Many families search for dental insurance with no waiting period when wisdom tooth pain becomes urgent. The assumption is that buying a new dental plan is the only way to avoid delays, but the truth is far more favorable.
Bone‑impacted extractions are medical procedures, and medical insurance cannot impose waiting periods for medically necessary surgery. Medicaid offers similar protections for children and many adults.
Only gum‑impacted extractions are covered under dental insurance rules, and timing and plan type determine whether immediate benefits apply. Understanding these distinctions helps families choose the fastest, most affordable path to care without unnecessary stress or expense.
🔍 1. Understanding Whether Your Wisdom Tooth Problem Is Medical or Dental
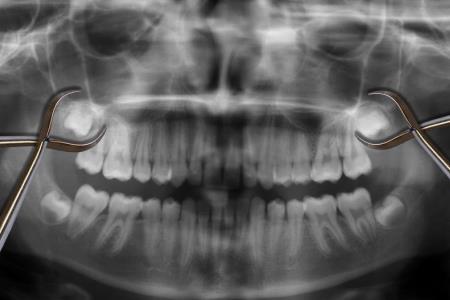
Many families don’t realize that wisdom tooth classification determines which insurance pays. The presence or absence of bone involvement changes everything about coverage timing and cost.
Bone‑Impacted Extractions Are Medical Procedures
Bone involvement shifts the extraction into the medical category, triggering rules that prohibit waiting periods for medically necessary surgery.
- Medical plans cover bony impactions, full impactions, and surgical extractions involving bone removal.
- Pre‑existing condition exclusions cannot apply to medically necessary surgery.
- Dental insurance never pays for bone‑impacted extractions.
- Oral surgeons bill medical claims using CPT codes and dental claims using CDT codes.
- Asking the surgeon to bill medical insurance often reduces out‑of‑pocket costs.
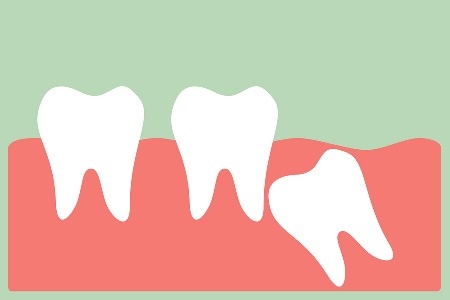
Gum‑Impacted Extractions Fall Under Dental Insurance
Gum‑impacted teeth are considered dental procedures, where waiting periods are common.
- Dental plans often impose 6–12‑month waiting periods for major services.
- Only certain plans offer immediate coverage for gum‑impacted extractions.
- Medical insurance rarely pays unless complications exist.
- Group dental plans may waive waiting periods depending on timing.
- Classification must be confirmed before choosing a coverage strategy.
Knowing whether your extraction is medical or dental clarifies which insurance applies and whether waiting periods matter. With that foundation in place, the next step is understanding how to secure medical coverage if you currently lack it.
🏥 2. Getting Medical Insurance If You Are Currently Uninsured
Families without medical insurance still have options for immediate coverage. Enrollment timing determines how quickly medically necessary surgery becomes covered.
ACA Medical Plans Cover Medically Necessary Surgery Immediately
Marketplace medical plans cannot delay coverage for medically necessary procedures, including bone‑impacted extractions.
- Coverage begins on the plan’s effective date.
- Pre‑existing conditions cannot be excluded or delayed.
- Deductibles and coinsurance still apply.
- Open Enrollment occurs annually for most applicants.
- Special Enrollment Periods allow mid‑year enrollment after qualifying events.
Eligibility Waiting Periods Apply Only to New Employees
Employer medical plans may require a short eligibility period before coverage begins.
- Federal law allows up to a 90‑day eligibility waiting period.
- Once active, medically necessary surgery is covered immediately.
- No additional waiting periods apply to bone‑impacted extractions.
- Coverage rules are uniform across employer plans.
- HR departments can confirm exact start dates.
Medical insurance offers the fastest path to coverage for bone‑impacted extractions, but Medicaid provides even broader protections for children and many adults. Understanding Medicaid rules reveals additional no‑wait opportunities.
📋 3. Medicaid Rules for Wisdom Tooth Removal
Medicaid coverage varies by age and state, but federal law guarantees immediate coverage for medically necessary care for children and many adults.
EPSDT Guarantees Full Coverage for Anyone Under Age 21
Federal EPSDT rules require states to cover all medically necessary wisdom tooth extractions for minors.
- Coverage includes bone‑impacted, gum‑impacted, and soft‑tissue impactions.
- No waiting periods or exclusions are permitted.
- States must cover treatment for pain, infection, or risk of harm.
- EPSDT rules apply uniformly across all states.
- Families can access care immediately once enrolled.
Adult Medicaid Coverage Depends on State Dental Benefits
Adults receive medical coverage for bone‑impacted extractions, while gum‑impacted coverage varies.
- All states cover medically necessary surgical extractions under the medical component.
- Adult dental benefits range from full coverage to emergency‑only.
- Gum‑impacted extractions may or may not be included.
- State Medicaid websites list covered dental services.
- Adults should verify benefits before scheduling care.
Retroactive Medicaid Can Cover Past Procedures
Many states offer retroactive coverage for recent medical and dental bills.
- Retroactive periods often extend up to 90 days.
- Eligibility depends on meeting Medicaid income rules.
- Retroactive coverage can reimburse past extractions.
- Applicants must document medical necessity.
- This option is unique to Medicaid programs.
Medicaid offers strong protections, especially for children and adults with bone‑impacted teeth. When gum‑impacted extractions require dental insurance, group dental plans become the next best opportunity for immediate benefits.
👥 4. Using Group Dental Plans When Timing Aligns
Group dental plans can provide immediate coverage for gum‑impacted extractions, but only when enrollment timing aligns with employer rules.
Scheduling Extractions at the Start of the New Plan Year
Open enrollment allows families to join group dental plans before the new plan year begins.
- Most employers hold open enrollment one to two months before the plan year.
- Coverage typically begins January 1 or the employer’s plan start date.
- Major services often have no waiting period for new plan‑year enrollees.
- Families can schedule extractions during the first month of coverage.
- This strategy works well for planned procedures.
Special Enrollment Periods Allow Immediate Mid‑Year Enrollment
Certain life events allow families to join group dental plans outside open enrollment.
- Qualifying events include losing job‑based coverage, marriage, or starting a new job.
- Aging off a parent’s plan at 26 also qualifies.
- Coverage begins immediately after enrollment is processed.
- Major services often start without waiting periods.
- SEP rules vary slightly by employer.
Large Employers Often Waive Waiting Periods for Major Services
Most large employer plans offer immediate coverage for major dental procedures.
- Waiting periods are uncommon in large group plans.
- Small employers may still impose waiting periods.
- Summary Plan Descriptions outline exact rules.
- HR departments can confirm waiting period policies.
- Families should request documentation before scheduling care.
Group dental plans help when timing aligns, but individual plans fill the gap when employer coverage is unavailable. Understanding how marketplace and private dental plans differ is essential for choosing immediate coverage.
👤 5. Individual Dental Insurance With No Waiting Period
Individual dental plans vary widely in waiting period rules, enrollment timing, and coverage for major services.
Marketplace Dental Plans Follow ACA Enrollment Rules
ACA dental plans differ for children and adults, affecting waiting periods and exclusions.
- Pediatric dental is an Essential Health Benefit with no waiting periods.
- Adult dental plans may impose waiting periods for major services.
- Pre‑existing condition exclusions, including missing tooth clauses, may apply.
- Preventive services typically have no waiting period.
- Some states prohibit waiting periods for adult dental plans.
Spirit Dental Offers Year‑Round Enrollment and Immediate Coverage
Spirit Dental is one of the few national carriers offering no‑wait major service coverage.
- Enrollment is available year‑round because it is not an ACA plan.
- Plans include graded benefits that increase annually.
- Immediate coverage applies to gum‑impacted extractions.
- In‑network discounts reduce surgeon fees significantly.
- High annual maximums support ongoing dental needs.
Choosing In‑Network Providers Reduces Total Costs
In‑network oral surgeons offer negotiated rates that lower out‑of‑pocket expenses.
- Network discounts apply even before insurance pays.
- Out‑of‑network providers may charge significantly more.
- Spirit Dental’s network varies by region.
- Families should confirm surgeon participation before scheduling.
- Network directories list participating providers.
Individual plans provide immediate options for gum‑impacted extractions, but emergencies require even faster solutions. Discount plans and financing help families manage urgent care needs without waiting.
💸 6. Immediate Options: Discount Plans and Financing
Urgent extractions require solutions that bypass enrollment windows and waiting periods entirely.
Dental Discount Plans Provide Instant Access to Lower Fees
Discount plans reduce the cost of extractions immediately after enrollment.
- No waiting periods or enrollment windows apply.
- Discounts typically range from 40–50% off standard fees.
- Plans activate the same day families enroll.
- Oral surgeons must participate in the discount network.
- Discount plans are ideal for urgent gum‑impacted extractions.
Financing Helps Spread Costs After Discounts Are Applied
Financing can follow discount enrollment to minimize upfront costs and smooth cash flow.
- Many oral surgeons offer third‑party financing options.
- Soft credit checks allow quick approval.
- Short‑term installment plans reduce upfront costs.
- Some lenders offer 0% promotional periods.
- Families should compare interest rates carefully.
Discount plans and financing help families manage urgent costs, but choosing the right path depends on the type of impaction and available insurance. A clear decision framework simplifies the process.
🛣️ 7. Choosing the Fastest Path to Coverage
Families can determine the best coverage strategy by identifying the type of impaction and available insurance options.
Decision Framework for Immediate Coverage
A simple comparison helps families choose the fastest, most affordable path.
- Bone‑impacted → medical insurance covers immediately.
- Under 21 → Medicaid covers all medically necessary extractions.
- Adults with bone‑impacted teeth → Medicaid medical component covers surgery.
- Gum‑impacted → group dental or Spirit Dental offer immediate options.
- No insurance → discount plan plus financing provides urgent access.
With a clear understanding of medical, Medicaid, group, and individual dental options, families can confidently choose the fastest path to affordable wisdom tooth removal.
Bottom Line
Most people searching for dental insurance with no waiting period already have immediate coverage through medical insurance or Medicaid. Gum‑impacted extractions require dental insurance, but group plans, Spirit Dental, and discount plans offer practical solutions depending on timing and urgency. Families who understand the difference between medical and dental classifications can avoid unnecessary delays and choose the most affordable path to care.
👤 About the Author
Kevin Haney, MBA, is a former health insurance agency owner with deep expertise in voluntary employee benefits, including dental insurance. As a stepfather to two adults with special needs, he brings a rare blend of professional insight and lived experience to navigating government programs such as Medicaid and overlooked financial strategies. His guidance helps families uncover practical ways to afford dental care with dignity and confidence.
Learn more